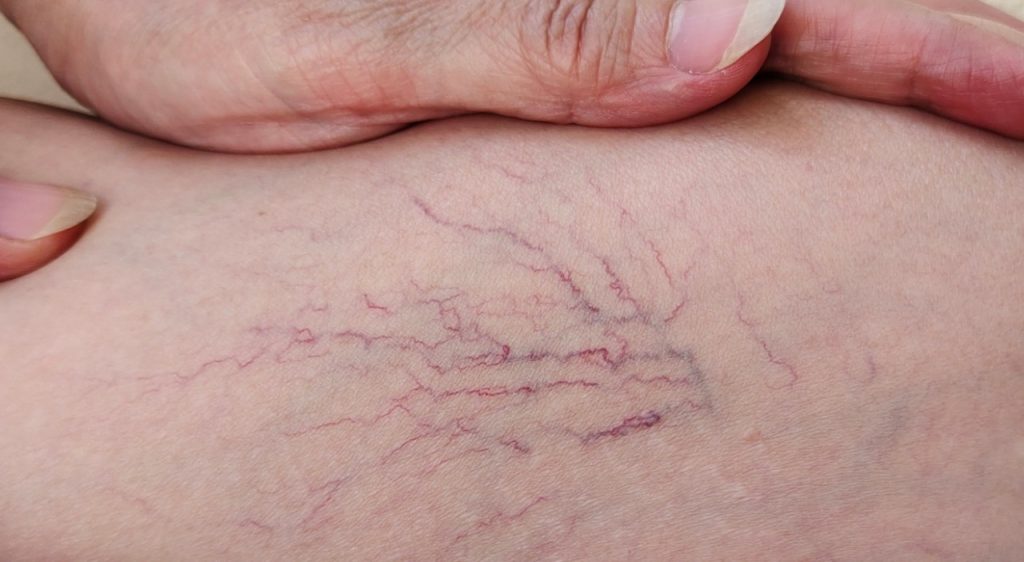
Spider veins—those fine red, blue, or purple clusters visible just beneath the skin—are common and usually harmless, but they can affect appearance and confidence. For online business owners, marketers, and other busy professionals who value efficient, results-driven solutions, understanding proven treatment options is essential.
This guide explains what spider veins are, why they develop, and when it makes sense to seek professional care. It also covers the most effective treatment and prevention strategies, including modern options for spider vein treatment in Round Rock, presented in clear, straightforward terms. The goal is to help readers make informed decisions quickly, without wading through unnecessary jargon.
What are Spider Veins?
Spider veins (telangiectasias) are small dilated blood vessels that appear near the surface of the skin. Unlike varicose veins, which are larger, raised, and sometimes painful, spider veins are typically flat, threadlike, and may form web-like patterns on the legs, face, or chest. They result from tiny valves in the veins failing to keep blood moving efficiently, causing capillaries and small veins to dilate.
Medically benign in most cases, spider veins can still create cosmetic concern and, for some people, a sensation of heaviness, itching, or mild discomfort. They’re visible indicators of underlying venous pressure or skin vascular changes. Understanding the difference between cosmetic and medical implications helps set realistic expectations for treatment: many procedures focus on improving appearance and symptom relief rather than treating systemic vascular disease.
Causes and Risk Factors
Several factors increase the likelihood of developing spider veins. Common contributors include:
- Genetics: A family history of spider or varicose veins is one of the strongest predictors. If parents or siblings have them, the probability rises substantially.
- Age: Veins lose elasticity, and valves weaken over time: spider veins become more common after middle age.
- Hormonal changes: Pregnancy, puberty, and menopause, and hormonal therapies like birth control, can influence vein dilation.
- Occupation and lifestyle: Prolonged standing or sitting, common in retail, office, and remote-work roles, raises venous pressure in the legs.
- Obesity and poor circulation: Extra body weight and low physical activity place stress on veins.
- Sun exposure and skin damage: Facial spider veins often correlate with chronic sun exposure, rosacea, or skin trauma.
Less common causes include prior blood clots, pelvic congestion, or localized trauma. For professionals balancing heavy workloads and irregular routines, awareness of these risk factors helps with prevention planning and early intervention.
When to Seek Treatment
Deciding when to seek treatment depends on symptoms, cosmetic concerns, and underlying health. Medical consultation is recommended if spider veins are accompanied by:
- Pain, swelling, cramping, or a heavy feeling in the legs
- Skin changes such as discoloration, ulcers, or persistent inflammation
- Rapid development of numerous new veins, or a history of blood clots
If the issue is mainly cosmetic, a consultation still helps determine the most efficient options and any contraindications. Busy entrepreneurs often prefer minimally disruptive treatments with fast recovery times. A vascular specialist or dermatologist can evaluate venous reflux (if suspected) with a simple duplex ultrasound and recommend targeted therapies. Early assessment avoids unnecessary procedures and ensures any contributing vascular conditions are identified.
Common Treatment Options
Treatment choice depends on vein size, location, symptoms, and patient preference. Below are the primary options clinicians use to reduce or remove spider veins.
Sclerotherapy: Procedure, Benefits, and Suitability
Sclerotherapy is the most widely used and evidence-backed treatment for spider veins on the legs. It involves injecting a sclerosant solution into the problematic vessels, causing them to collapse and gradually fade over weeks to months. Key points:
- Procedure: Typically performed in an outpatient setting. Multiple injections may be needed across sessions. Each session lasts about 15–45 minutes, depending on the area treated.
- Benefits: High success rate for small to medium-sized spider veins, minimal downtime, and quick return to normal activities. Compression stockings are usually recommended afterward to support healing.
- Suitability: Best for leg spider veins: not always ideal for facial spider veins or very tiny capillaries. People with certain medical conditions, like active clotting disorders, may not be candidates.
Sclerotherapy often delivers a good balance between effectiveness and convenience for professionals who want visible improvement without major disruption.
Laser and Light-Based Therapies: Types and Outcomes
Laser and intense pulsed light (IPL) therapies target the pigment in blood vessels, heating and collapsing them. They are especially useful for facial spider veins and small capillaries.
- Types: Surface lasers (pulsed dye laser, KTP) and transdermal devices (Nd:YAG) are commonly used. Each has strengths depending on skin tone and vessel depth.
- Limitations: Laser can cause temporary redness, hyperpigmentation, or, rarely, blistering, particularly on darker skin tones. Proper device selection and experienced clinicians mitigate risks.
For professionals seeking quick, in-office treatments with no needles for facial areas, laser options are attractive, just ensure realistic expectations about repeat sessions.
Ambulatory Phlebectomy and Other In-Office Procedures
Ambulatory phlebectomy is a minor surgical technique used for larger superficial veins. Tiny incisions allow the removal of affected segments under local anesthesia.
- Use case: Larger bulging veins not suitable for sclerotherapy or when cosmetic contouring is desired.
- Recovery: Short; most people return to daily activities quickly, with some bruising and numbness at incision sites.
- Alternatives: Radiofrequency or endovenous laser ablation treat incompetent larger veins when reflux is present: these are more invasive but effective for deeper pathology.
These options are less common for classic spider veins but essential in a comprehensive venous treatment pathway when multiple vein types coexist.
Topical Treatments and At-Home Care: What Works
Topical creams claim to reduce the appearance of spider veins, but evidence is limited. Ingredients like vitamin K, retinoids, and certain plant extracts may improve skin appearance but won’t eliminate underlying dilated vessels. Practical at-home measures include:
- Daily sunscreen to prevent worsening
- Regular exercise and leg elevation to improve circulation
- Compression stockings after procedures to optimize results and reduce recurrence
For many, at-home care complements clinical treatments rather than replacing them. Busy professionals should view topical products as supportive maintenance rather than primary therapy.
Preparing for Treatment and What to Expect
A clear pre-treatment plan reduces stress and improves outcomes. Preparation and realistic expectations are key for anyone balancing treatment with work commitments.
Preprocedure Assessment and Questions to Ask
Before any procedure, a consultation typically covers medical history, medication review (blood thinners may need discussion), and an examination. Recommended questions include:
- Is a duplex ultrasound needed to check for deeper venous reflux?
- Which treatment is best for my vein type and skin tone?
- How many sessions are likely, and what are the expected costs?
- What downtime should be anticipated, and when can normal work resume?
- What are the common side effects and signs that require follow-up?
A concise, prioritized question list helps busy clients get the answers they need in one visit or call.
Recovery Timeline, Side Effects, and Follow-Up Care
Recovery is usually brief. Typical expectations:
- Immediate: Mild soreness, redness, or bruising: compression stockings or bandages may be advised.
- Short term (1–2 weeks): Discoloration and bruising fade; many return to normal activities the same day or within a few days.
- Follow-up: Providers often schedule a follow-up 4–12 weeks after treatment to assess results and plan additional sessions if needed.
Serious complications are rare but include deep vein thrombosis, infection, or persistent pigmentation. Prompt medical attention is important if unusual symptoms occur.
Results Timeline and When to Consider Repeat Treatment
Visible improvement varies by treatment: sclerotherapy and lasers typically show fading within 3–12 weeks, while complete cosmetic clearance may take several months and multiple sessions. Some veins respond fully; others diminish partially and need touch-ups. Recurrence can happen, especially if the underlying venous reflux isn’t treated. A staged approach, treating the most visible veins first and reassessing, often yields the best balance of results and cost-efficiency.
Prevention and Long-Term Maintenance
Preventing new spider veins and maintaining results is a long-term effort that pairs medical care with daily habits. For professionals who travel frequently or sit for long periods, small adjustments make a measurable difference.
Lifestyle Changes and Habits to Reduce Recurrence
Effective habits include:
- Move regularly: Take brief walks every hour during long workdays to stimulate circulation.
- Maintain a healthy weight: Even modest weight loss reduces venous pressure.
- Exercise: Low-impact aerobic activities, walking, cycling, swimming support vascular health.
- Avoid prolonged immobility: On long flights, compressive stockings and occasional leg movement reduce risk.
These strategies not only help veins but also support overall cardiovascular health, an efficient, high-return investment for busy people.
Skincare, Compression, and Professional Follow-Up
Sunscreen and gentle skincare protect facial vessels: retinoids and professional skin treatments can enhance skin texture and tone. For leg maintenance, compression stockings after treatment and during long periods of standing or travel are a staple recommendation. Periodic check-ins with a vascular specialist or dermatologist ensure new veins are addressed early, and any underlying reflux is monitored. Scheduling these follow-ups as part of annual health tasks makes compliance easier for those with packed calendars.
Conclusion
Spider vein treatment delivers both cosmetic and symptomatic benefits when chosen to fit the vein type, skin tone, and lifestyle. For online business owners and marketers who value time and outcomes, minimally invasive options like sclerotherapy and targeted laser treatments offer efficient paths to clearer, healthier-looking skin with limited downtime. Prevention, through movement, weight management, sun protection, and compression, reduces recurrence and extends results. A brief consultation with a qualified specialist helps prioritize treatments, set realistic expectations, and align care with personal schedules. With the right approach, clearing visible veins can be straightforward and compatible with a busy professional life.